Factors associated with poor colonoscopy preparation
DOI:
https://doi.org/10.22516/25007440.1001Keywords:
Colonoscopia, Calidad de la preparación, Factores de riesgo relacionados con la preparación, Escalas de preparaciónAbstract
Introduction: Good bowel preparation is essential for a quality colonoscopy. Thus, evaluating the risk factors associated with poor preparation is necessary. This problem has not been widely addressed in Colombia.
Aim: To identify the factors associated with poor intestinal preparation.
Materials and methods: Observational, analytical, cross-sectional, multicenter study in patients > 18 years of age who underwent colonoscopy and attended gastroenterology services between January and June 2020 in Bogotá. A Boston scale > 6 was defined as good preparation, and a Boston scale ≤ 6 was defined as poor preparation.
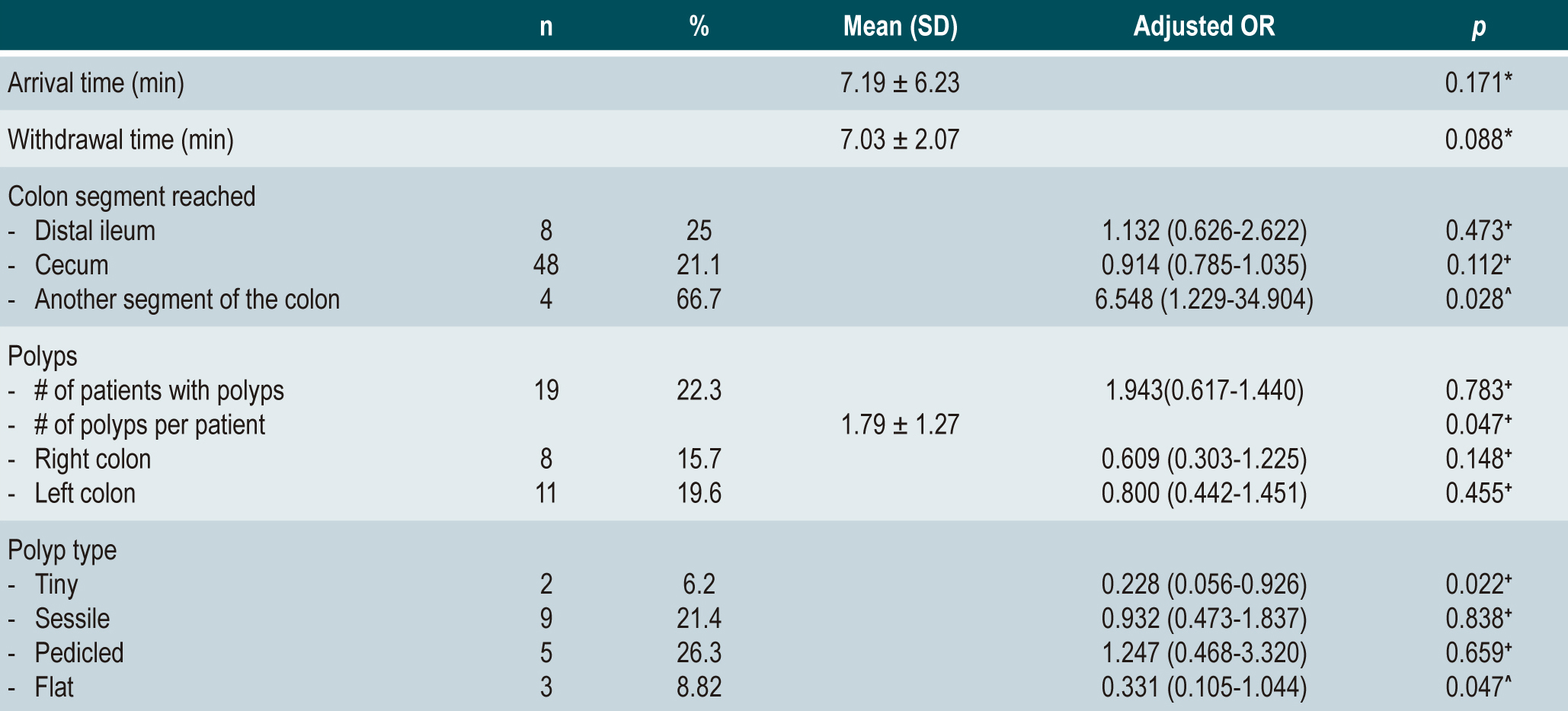
Results: 265 patients were included, of whom 205 (77.4%) were well prepared and 60 (22.6%) had inadequate preparation. Factors associated with poor bowel preparation were age older than 60 years (odds ratio [OR]: 1.359; 95% confidence interval [CI]: 1.059-1.745; p = 0.026); male sex (OR: 1.573; 95% CI: 1.128-2.194; p = 0.012); obesity (BMI > 30 kg/m2; OR: 2.539; 95% CI: 1.388-4.645; p = 0.002); constipation (OR: 1.924; 95% CI: 1.154-3.208; p = 0.014); the use of antidepressants (OR: 2.897; 95% CI: 1.199-6.997; p = 0.014) and calcium antagonists (OR: 2.445; 95% CI: 1.292-4.630; p = 0.005), and having abdominopelvic surgeries (OR: 1.325 95% CI: 1.042-1.684, p = 0.034). Regarding the procedure, there was less polyp detection per patient (p = 0.04) and less minute (p = 0.020) and flat (p = 0.047) polyp detection in the poor bowel preparation group.
Conclusions: This is the first study in Colombia in which the factors associated with poor intestinal preparation are described and include variables not explored in other studies. The results found are similar to those reported in the literature. These studies should be promoted with more patients, establishing a score for predicting poor preparation.
Downloads
References
Siegel R, Miller K, et al. Colorectal cancer statistics; CA Cancer J Clin 2020;70(3):145-164. https://doi.org/10.3322/caac.21601
Cortés A, Bravo L, et al. Colorectal cancer incidence, mortality and survival in Cali, Colombia, 1962-2012. 2014;56(5):457-64. https://doi.org/10.21149/spm.v56i5.7371
Bravo L, García L; et al. Reliable information for cancer control in Cali, Colombia. Colomb medica. 2018;49(1):23-34. https://doi.org/10.25100/cm.v49i1.3689
Govani S, Elliott E, et al. Predictors of suboptimal bowel preparation in asymptomatic patients undergoing average-risk screening colonoscopy. World J Gastrointest Endosc. 2016;8(17):616. https://doi.org/10.4253/wjge.v8.i17.616
Guo X, Shi X, et al. Risk Factors Associated with Inadequate Bowel Preparation in Patients with Functional Constipation. Dig Dis Sci. 2020;65(4):1082-91. https://doi.org/10.1007/s10620-019-05847-5
Mahmood S, Farooqui SM, Madhoun MF. Predictors of inadequate bowel preparation for colonoscopy: A systematic review and meta-analysis. Eur J Gastroenterol Hepatol. 2018;30(8):819-26. https://doi.org/10.1097/MEG.0000000000001175
Lieberman D, Ladabaum U, et al. Screening for Colorectal Cancer and Evolving Issues for Physicians and Patients: A Review. JAMA. 2016;316(20):2135-45. https://doi.org/10.1001/jama.2016.17418
Zhu L, MingMing Z, et al. Enhanced education for bowel preparation before colonoscopy: a state-of-the-art review. J Dig Dis. 2017;18(2):84-91. https://doi.org/10.1111/1751-2980.12446
Pellisé M. Colonoscopia en el cribado, seguimiento y tratamiento del cáncer colorrectal y sus lesiones precursoras. Gastroenterol Hepatol. 2015;388(1):71-7. https://doi.org/10.1016/S0210-5705(15)30022-4
Dekker E, Tanis PJ, et al. Colorectal cancer. Lancet 2019;394(10207):1467-80. https://doi.org/10.1016/S0140-6736(19)32319-0
Parekh PJ, Oldfield EC, Johnson DA. Bowel preparation for colonoscopy: What is best and necessary for quality? Curr Opin Gastroenterol. 2019;35(1):51-7. https://doi.org/10.1097/MOG.0000000000000494
Hassan C, East J, Radaelli F et al. Bowel preparation for colonoscopy: European society of gastrointestinal endoscopy (ESGE) guideline-update 2019. Endoscopy. 2019;51(8):775-94. https://doi.org/10.1055/a-0959-0505
Zhang Y, Niu M et al. The incidence of and risk factors for inadequate bowel preparation in elderly patients: A prospective observational study. Saudi J Gastroenterol. 2018;24(2):87-92. https://doi.org/10.4103/sjg.SJG_426_17
Gimeno A, Baute J et al. Risk factors for inadequate bowel preparation: A validated predictive score. Endoscopy. 2017;49(6):536-43. https://doi.org/10.1055/s-0043-101683
Jhonson D, Barkun A, Cohen L, et al. Optimizing adequacy of bowel cleansing for colonoscopy: recommendations from the US multi-society task force on colorectal cancer. Gastroenterology. 2014;1147(4):903-24. https://doi.org/10.1053/j.gastro.2014.07.002
Kastenberg D, Bertiger G, Brogadir S. Bowel preparation quality scales for colonoscopy. World J Gastroenterol. 2018;24(26):2833-43. https://doi.org/10.3748/wjg.v24.i26.2833
Fanjul I, Lasa J, et al. Factores relacionados al paciente que afectan la limpieza del colon previo a la colonoscopía. Acta Gastroenterol Latinoam. 2016;46(1):18-21.
Garber A, Sarvepalli S, et al. Modifiable factors associated with quality of bowel preparation among hospitalized patients undergoing colonoscopy. Vol. 14, Journal of Hospital Medicine. 2019: 278-83. https://doi.org/10.12788/jhm.3173
Bugajski M, WIeszczy P, et al. Modifiable factors associated with patient- reported pain during and after screening colonoscopy. Gut. 2018;67(11):1958-64. https://doi.org/10.1136/gutjnl-2017-313905
Anderson JC, Baron JA, et al. Factors Associated With Shorter Colonoscopy Surveillance Intervals for Patients With Low-Risk Colorectal Adenomas and Effects on Outcome. Gastroenterology. 2017 ;152(8):1933- 1943.e5. https://doi.org/10.1053/j.gastro.2017.02.010
Harewood G, Sharma V, Garmo P. Impact of colonoscopy preparation quality on detection of suspected colonic neoplasia. Gastrointest. Endosc.2003 58(1):76-9. https://doi.org/10.1067/mge.2003.294
Sulz M, Kroger A, et al. Meta-Analysis of the Effect of Bowel Preparation on Adenoma detection: Early adenomas affected stronger than advanced adenomas. PLoS One .2016;6:11 https://doi.org/10.1371/journal.pone.0154149
Clark BT, Protiva P et al. Quantification of Adequate Bowel Preparation for Screening or Surveillance Colonoscopy in Men. Gastroenterology. 2016 Feb 1;150(2):396-405. https://doi.org/10.1053/j.gastro.2015.09.041
Dik VK, Moons LMG, et al. Predicting inadequate bowel preparation for colonoscopy in participants receiving split-dose bowel preparation: Development and validation of a prediction score. Gastrointest Endosc. 2015;81(3):665-72. https://doi.org/10.1016/j.gie.2014.09.066
Paik N, Kim ER, et al. Usefulness of personal bowel habits as a predictive factor for inadequate bowel preparation for colonoscopy: A prospective questionnaire-based observational study. Gut and Liver. 2019; 13:169-75. https://doi.org/10.5009/gnl18236
Wong MCS, Ching JYL, et al. Determinants of bowel preparation quality and its association with adenoma detection: A prospective colonoscopy study. Med (United States). 2016;95(2):1-8. https://doi.org/10.1097/MD.0000000000002251
Amitay EL, Niedermaier T et al. Risk factors of inadequate bowel preparation for screening colonoscopy. J Clin Med. 2021;10(12):2740. https://doi.org/10.3390/jcm10122740
Gandhi K, Tofani C, et al. Patient characteristics associated with quality of colonoscopy preparation: A systematic review and meta-analysis. Clin Gastroenterol Hepatol.2018;16(3):357-369.e10. https://doi.org/10.1016/j.cgh.2017.08.016
Hassan C, Fuccio L, Bruno M, et al. A predictive model identifies patients most likely to have inadequate bowel preparation for colonoscopy. Clin Gastroenterol Hepatol. 2012;10(5):501-6. https://doi.org/10.1016/j.cgh.2011.12.037
Gralnek IM, Hassan C, et al. ESGE and ESGENA Position Statement on gastrointestinal endoscopy and the COVID-19 pandemic. Endoscopy. 2020;52(6):483-90. https://doi.org/10.1055/a-1155-6229
Yadlapati R, Jhonston E et al. Predictors of inadequate inpatient colonoscopy preparation and its association with Hospital length of stay and costs. Dig Dis Sci.2015; 60(11):3482-90. https://doi.org/10.1007/s10620-015-3761-2
Doykov D, Andonov V, et al; Risk factors and incidence of poor bowel preparation in elderly patients: Prospective Study. 2019; 61:370-6. https://doi.org/10.3897/folmed.61.e39409
Fitzpatrick-Lewis D, Ali MU, Warren R, et al. Screening for colorectal cancer: A systematic review and meta-Analysis. Clin colorectal cancer. 2016;15(4):298-313. https://doi.org/10.1016/j.clcc.2016.03.003
Repici A, Badalamenti M, et al. Efficacy of real-time computer-aided detection of colorectal neoplasia in a randomized trial. Gastroenterology. 2020;159(2):512-520.e7. https://doi.org/10.1053/j.gastro.2020.04.062
Lebwohl B, Kastrinos F, et al. The impact of suboptimal bowel preparation on adenoma miss rates and the factors associated with early repeat colonoscopy. Gastrointest Endosc. 2011 Jun;73(6):1207-14. https://doi.org/10.1016/j.gie.2011.01.051
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2023 Revista colombiana de Gastroenterología

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
Aquellos autores/as que tengan publicaciones con esta revista, aceptan los términos siguientes:
Los autores/as ceden sus derechos de autor y garantizarán a la revista el derecho de primera publicación de su obra, el cuál estará simultáneamente sujeto a la Licencia de reconocimiento de Creative Commons que permite a terceros compartir la obra siempre que se indique su autor y su primera publicación en esta revista.
Los contenidos están protegidos bajo una licencia de Creative Commons Reconocimiento-NoComercial-SinObraDerivada 4.0 Internacional.


| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |














