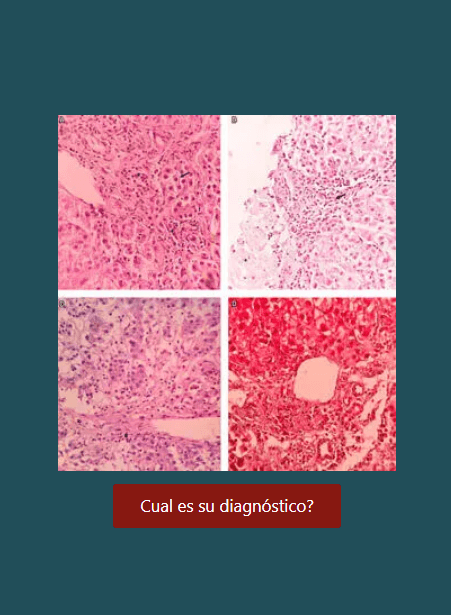
Sweet syndrome to peritoneal tuberculosis: Case report
DOI:
https://doi.org/10.22516/25007440.528Keywords:
peritoneal, tuberculosis, Sweet syndrome, ADA, CA-125Abstract
Peritoneal tuberculosis is a rare disease that accounts for 25-50% of abdominal tuberculosis cases and 0.1-0.7% of all cases of tuberculosis. Mortality is 35% when treatment is delayed, and 73% in patients with cirrhosis. It also has a wide clinical spectrum, so its differential diagnosis covers conditions such as cirrhosis, malignancy, nephrotic syndrome, and malnutrition. Moreover, imaging studies may reveal peritoneal metastases; carcinomatosis of gastric, pancreatic, bladder, ovarian, colonic origin; and infectious diseases such as actinomycosis, coccidioidomycosis, histoplasmosis or non-tuberculous mycobacteria. Diagnosis is initially supported by blood chemistry, liver and renal function tests, ultrasound, CT scans, paracentesis with peritoneal fluid cytochemistry, and ADA and PCR measurement. The gold standard is laparoscopy with peritoneal biopsy and pathological or microbiological confirmation. Cases of false negatives of the ADA test have been described in immunosuppression or use of antituberculosis drugs. Monitoring of disease activity by measuring CA-125 levels has been considered. The following is the report of an unusual case of peritoneal TB with secondary Sweet’s syndrome, in which the ADA report was initially negative, possibly due to meropenem administration, and in whom disease activity was monitored through Ca125. False negative reports of ADA and Sweet’s secondary to TB are very rare, so this case contributes to the literature on these conditions.
Downloads
References
Organización Mundial de la Salud. [Internet]. Informe mundial sobre la tuberculosis (Sinopsis); 2019. p. 1-8. Disponible en: https://www.who.int/tb/publications/global_report/gtbr2019_ExecutiveSummary_es.pdf
Wu DC, Averbukh LD, Wu GY. Diagnostic and Therapeutic Strategies for Peritoneal Tuberculosis: A Review. J Clin Transl Hepatol. 2019;7(2):140-148. https://doi.org/10.14218/JCTH.2018.00062.
Zumla A, Raviglione M, Hafner R, von Reyn CF. Tuberculosis. N Engl J Med. 2013;368(8):745-55. https://doi.org/10.1056/NEJMra1200894
Tang LC, Cho HK, Wong Taam VC. Atypical presentation of female genital tract tuberculosis. Eur J Obstet Gynecol Reprod Biol. 1984;17(5):355-63. https://doi.org/10.1016/0028-2243(84)90115-1
Getahun H, Matteelli A, Chaisson RE, Raviglione M. Latent Mycobacterium tuberculosis infection. N Engl J Med. 2015;372(22):2127-35. https://doi.org/10.1056/NEJMra1405427
Karmakar PS, Sherpa PL, Ray AN, Saha BK, Santra T, Saha S, Chakrabarti I. Sweet’s syndrome: a very rare association with pulmonary tuberculosis. J Infect Dev Ctries. 2013;7(5):417-20. https://doi.org/10.3855/jidc.2606
Rodríguez L, Yurgaky J, Otero W, Faizal M. Síndromes paraneoplásicos en tumores gastrointestinales. Revisión de tema. Rev Colomb Gast. 2017;32(3):230-44. https://doi.org/10.22516/25007440.155
Baquero J, Garlatti L, Torre A. Síndrome de Sweet asociado a síndrome mielodisplasico. Rev. Hosp Ital B. Aires. 2015;35(2):62-65.
Mamlouk M, vanSonnenberg E, Shankar S, Silverman S. Omental Cakes: unusual aetiologies and CT appearances. Insights Imaging. 2011;2(4):399-408. https://doi.org/10.1007/s13244-011-0105-4
Balteiro A, Carrión E. Diagnóstico de la Ascitis. Gastroenterología y Hepatología continuada. 2008;7(1):6-10.
https://doi.org/10.1016/S1578-1550(08)72976-0
Boyer TD. Diagnosis and management of cirrhotic ascites. En: Zakim, Boyer DT. (editores). Hepatology: A Textbook of Liver Disease. 4.a edición. Filadelfia: Saunders; 2003. p. 1227-1232.
Riquelme A, Calvo M, Salech F, Valderrama S, Pattillo A, Arellano M, Arrese M, Soza A, Viviani P, Letelier LM. Value of adenosine deaminase (ADA) in ascitic fluid for the diagnosis of tuberculous peritonitis: a meta-analysis. J Clin Gastroenterol. 2006;40(8):705-10. https://doi.org/10.1097/00004836-200609000-00009
Yoon YJ, Ahn SH, Park JY, Chon CY, Kim DY, Park YN, Han KH. What is the role of diagnostic laparoscopy in a gastroenterology unit? J Gastroenterol. 2007;42(11):881-6. https://doi.org/10.1007/s00535-007-2106-0
van Rijn SP, Zuur MA, Anthony R, Wilffert B, van Altena R, Akkerman OW, de Lange WCM, van der Werf TS, Kosterink JGW, Alffenaar JC. Evaluation of Carbapenems for Treatment of Multi- and Extensively Drug-Resistant Mycobacterium tuberculosis. Antimicrob Agents Chemother. 2019;63(2):e01489-18. https://doi.org/10.1128/AAC.01489-18
Yilmaz A, Ece F, Bayramgürler, Akkaya E, Baran R. The value of CA-125 in the evaluation of the tuberculosis activity. Respir Med. 2001;95(8):666-69. https://doi.org/10.1053/rmed.2001.1121
Gómez AA. Tuberculosis peritoneal con niveles elevados de CA-125. Rev Fac Med U Jav Colomb. 2013;61(3):311-14.
Oey RC, van Buuren HR, de Man RA. The diagnostic work-up in patients with ascites: current guidelines and future prospects. Neth J Med. 2016;74(8):330-35.
Fei GJ, Zhang LF, Shu HJ. Values of different laboratory diagnostic approaches for tuberculous peritonitis. Zhongguo Yi Xue Ke Xue Yuan Xue Bao. 2018;40(4):534-38.
Pimkina E, Zablockis R, Nikolayevskyy V, Danila E, Davidaviciene E. The Xpert MTB/RIF assay in routine diagnosis of pulmonary tuberculosis: A multicentre study in Lithuania. Respir Med. 2015;109(11):1484-89. https://doi.org/10.1016/j.rmed.2015.07.006
Raj A, Singh N, Gupta KB, Chaudhary D, Yadav A, Chaudhary A, Agarwal K, Varma-Basil M, Prasad R, Khuller GK, Mehta PK. Comparative Evaluation of Several Gene Targets for Designing a Multiplex-PCR for an Early Diagnosis of Extrapulmonary Tuberculosis. Yonsei Med J. 2016;57(1):88-96. https://doi.org/10.3349/ymj.2016.57.1.88
Runyon BA, Hoefs JC, Morgan TR. Ascitic fluid analysis in malignancyrelated ascites. Hepatology. 1988;8(5):1104-9. https://doi.org/10.1002/hep.1840080521
Sanai FM, Bzeizi KI. Systematic review: tuberculous peritonitis-presenting features, diagnostic strategies and treatment. Aliment Pharmacol Ther. 2005;22(8):685-700. https://doi.org/10.1111/j.1365-2036.2005.02645.x
Ramappa V, Aithal GP. Hepatotoxicity related to anti-tuberculosis drugs: Mechanisms and management. J Clin Exp Hepato. 2013;3(1):37-49. https://doi.org/10.1016/j.jceh.2012.12.001
Downloads
Published
How to Cite
Issue
Section
License
Aquellos autores/as que tengan publicaciones con esta revista, aceptan los términos siguientes:
Los autores/as ceden sus derechos de autor y garantizarán a la revista el derecho de primera publicación de su obra, el cuál estará simultáneamente sujeto a la Licencia de reconocimiento de Creative Commons que permite a terceros compartir la obra siempre que se indique su autor y su primera publicación en esta revista.
Los contenidos están protegidos bajo una licencia de Creative Commons Reconocimiento-NoComercial-SinObraDerivada 4.0 Internacional.


| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |